
Created by - Rigomo Team
Esophageal Foreign Bodies – Gastrointestinal Disorders
80% of patients with esophageal foreign bodies are children. Usually, a caregiver will bring the child to the ED after seeing them eat anything. The diagnosis may be challenging if the ingestion was not seen.CLINICAL FEATURES1. Symptomsa) Adults typically complain of a foreign body sensation in the throat or chest. The patient may appear anxious and experience retching or vomiting, choking, coughing, or drooling.b) Children: Symptoms include refusal to eat, increased salivation, pain on swallowing, vomiting, choking, and referred respiratory symptoms (e.g., stridor, cough, and wheezing).2. Physical examination may reveal signs of infection. Fever and/or subcutaneous emphysema in the neck is suggestive of esophageal perforation.EVALUATION1. Laryngoscopy: Direct or indirect laryngoscopy may be performed if the patient feels that the foreign body is in the throat or if respiratory symptoms are present.2. Radiographya) Radiographs can be used to pinpoint the location of radiopaque objects (e.g., coins, button batteries, sharp objects).b) Pneumomediastinum or air in the soft tissues suggests perforation.3. Endoscopy also allows localization of the object and is often therapeutic.4. Esophagraphy: An esophagram should be performed only after consulting with a specialist because the contrast material may interfere with later attempts at endoscopy.THERAPY1. Coins and small smooth objects often pass through the gastrointestinal tract without difficulty. Coins that are too large to pass are removed by endoscopy. They can also be removed, by experienced physicians, using a Foley catheter guided by fluoroscopy.2. Button batteries have the potential to cause chemical corrosion and perforation of the esophagus and must be endoscopically removed as soon as possible.3. Sharp objects must be removed by endoscopy.4. Food impactions can be treated expectantly if the patient is managing his or her secretions adequately. Medical interventions include the following:a) Glucagon (1 mg intravenously) may relieve the impaction. A second 2-mg dose can be administered in 20 minutes if the first dose is ineffective.b) Nitroglycerin (administered sublingually) may also assist in relieving the impaction.c) Nifedipine (10 mg sublingually) relaxes the lower esophageal sphincter and may allow passage of the food bolus.d) Diazepam may be used as a last resort.e) Endoscopy should be performed if the bolus has not passed after several hours.DISPOSITION: In order to rule out underlying esophageal pathology, all patients require follow-up.
More detailsPublished - Fri, 04 Nov 2022
Created by - Rigomo Team
Hypomagnesemia: Clinical Features, Evaluation & Treatment
Hypomagnesemia occurs when the serum magnesium concentration falls below 1.0 mEq/L.CLINICAL FEATURES1. Symptoms: Malaise, diffuse weakness, anorexia, nausea, vomiting, and seizures2. Physical examination findings: Mimic findings of hypocalcemia, with nervous system complaints dominating the clinical picture. Chvostek sign, Trousseau sign, tremors, twitching, clonus, increased deep tendon reflexes, carpopedal spasm, frank tetany, delirium, movement disorders, and dysarthriaEVALUATION1. Laboratory studies include serum magnesium, calcium, BUN, creatinine, and glucose levels and a serum electrolyte panel.2. Electrocardiography: ECG findings include atrial and ventricular tachyarrhythmias, torsades de pointes, and a prolonged QT interval. Arrhythmias caused by hypomagnesemia may not respond to the usual antiarrhythmic therapy, but they may respond well to intravenous magnesium. Magnesium (2 g) should be administered rapidly over 2 minutes via an intravenous line to patients with pulseless ventricular tachycardia suspected of being hypomagnesemia (e.g., a patient with myocardial infarction who is taking diuretics).3. Ancillary tests (e.g., radiographs) may be required to diagnose the underlying cause.THERAPY1. Mild hypomagnesemia: Oral supplementation. Magnesium hydroxide (200 to 600 mg, four times daily) is usually used.2. Severe hypomagnesemia: Marked neurologic manifestations or malignant ventricular arrhythmias is treated with 2 to 4 g of magnesium sulfate administered in 100 to 200 mL of 5% dextrose in water over 20 minutes. Additional treatment should be directed toward correcting the underlying cause of hypomagnesemia.DISPOSITION: Indications for admission include a serum magnesium level below 1 mEq/L, severe central neurologic manifestations, cardiac arrhythmias, and severe underlying disorders.
More detailsPublished - Sat, 05 Nov 2022

Created by - Rigomo Team
Hypermagnesemia: Causes, Clinical Features & Treatment
Serum magnesium level greater than 2.5 mEq/LCAUSES: Because the kidney is efficient in excreting excess magnesium, hypermagnesemia is uncommon except in the presence of renal failure or an iatrogenic cause. Other causes of hypermagnesemia include rhabdomyolysis, tumor lysis, burns, tissue trauma, diabetic ketoacidosis, hypothyroidism, cathartic abuse, antacids, preeclampsia or eclampsia treatment, and adrenal insufficiency.CLINICAL FEATURES1. Symptoms: Nausea, vomiting, lethargy, mental confusion, and coma2. Physical examination findings: When the magnesium level exceeds 4 mEq/L. Depression of the deep tendon reflexes, marked muscle weakness, bulbar paralysis, and respiratory insufficiency.EVALUATION1. Laboratory studies include serum calcium, ionized calcium, BUN, and creatinine levels and a serum electrolyte panel. 2. Electrocardiography: Dysrhythmias and cardiac arrest can occur at serum magnesium levels exceeding 8mEq/L, but the ECG manifestations of hypermagnesemia are variable and nonspecific.THERAPY1. Exogenous sources of magnesium should be removed.2. Pharmacologic therapya) Calcium gluconate or calcium chloride: Because calcium transiently reverses the effects of hypermagnesemia by acting as a direct antagonist, 10 mL of 10% calcium gluconate or calcium chloride solution can be given intravenously in symptomatic patients.b) Furosemide: In patients with normal renal function, brisk diuresis with intravenous normal saline and furosemide will enhance urinary magnesium excretion.3. Dialysis: In patients with very high magnesium levels or patients with renal failure, emergency peritoneal dialysis or hemodialysis may be required.DISPOSITION: Patients with magnesium levels above 8 mEq/L require admission to a monitored bed and should be considered for early dialysis.
More detailsPublished - Tue, 08 Nov 2022

Created by - Rigomo Team
Non-ketotic Hyperosmolar Coma
The syndrome is characterized by severe hyperglycemia, hyperosmolarity, and dehydration. Non-ketotic hyperosmolar coma is less common than diabetic ketoacidosis and commonly occurs as an early manifestation of non–insulin-dependent diabetes.ETIOLOGY1. Patients with diabetes who have been subjected to a stressor (e.g., infection, stroke, gastrointestinal bleeding, pancreatitis) or who are taking thiazide diuretics, corticosteroids, phenytoin, cimetidine, propranolol, or calcium channel blockers may develop nonketotic hyperosmolar coma.2. Non-diabetic patients: Situations that cause severe dehydration or excessive glucose load (e.g., burns, heat stroke, peritoneal dialysis, hemodialysis, and the ingestion of enormous amounts of sugar-containing foods) may cause this disorder in patients without diabetes.PATHOGENESIS: Non-ketotic hyperosmolar coma and diabetic ketoacidosis represent different ends of a spectrum of lipid mobilization. Non-ketotic hyperosmolar coma is precipitated by stress that increases glucose levels over days or weeks. It is believed that a tiny dose of insulin will decrease ketogenesis. Osmotic diuresis that is significantly results in severe dehydration and altered mental status.CLINICAL FEATURES1. Patient history: Most patients are elderly with either non–insulin-dependent diabetes (67% of patients) or insulin-dependent diabetes (33% of patients).2. Symptoms: Patients develop polydipsia and polyuria initially, followed by alterations in mental status. Before a stupor and coma set in, the illness can go undetected.3. Physical examination findings: Dehydration, fever, hypotension, tachycardia, and a variety of breathing patterns are the main findings. Neurologic symptoms can include tremors, fasciculations, hemisensory abnormalities, and hemiparesis.DIFFERENTIAL DIAGNOSES: Any disorder that can cause altered mental status (e.g., hepatic failure, uremia, sepsis, stroke, drug ingestion, lactic acidosis) must be considered.EVALUATION1. The values of measured and calculated serum osmolarity, glucose, and ketones are critical.a) Usually, the glucose level is 1,000 mg/dL or above.b) Although ketones may be present in small amounts, there is usually an absence of ketonemia and ketonuria.c) Over 350 mOsm/kg or more describe the serum osmolarity.2. Serum electrolyte, BUN, and creatinine levels; urinalysis; and venous blood gas determinations are indicated.a) Serum sodium ranges from 120 to 160 mEq/L, and potassium depletion is usually severe.b) Typically, the BUN is increased and the BUN:creatinine ratio is greater than 30:1.3. Other studies: Finding the root of the problem is crucial. It may be necessary to perform a lumbar puncture, chest radiograph, ECG, computed tomography head scan, or cultures.THERAPY1. Fluid resuscitation: The average fluid deficit is 8 to 12 L; therefore, administration of half-normal saline (or normal saline for hypotensive patients) is indicated. The patient's hydration deficit should be filled in during the course of the first 12 hours, followed by the final 24 hours.2. Replacement of potassium should begin early in the therapeutic process. If the patient's fluid status is such that he or she is able to produce urine, an infusion is typically started at a rate of 10 to 20 mEq/L for the first 24 to 36 hours.3. Continuous infusion of insulin is used (0.1 U/kg/hour). As soon as the blood glucose level exceeds 300 mg/dL, the insulin should be stopped.4. If the glucose level is under 250 mg/dL, glucose is indicated.5. Phosphate: Administration of phosphate is controversial.6. For the prevention of venous and arterial thrombosis, low-dose heparin may be administered.DISPOSITION: A significant death rate is linked to non-ketotic hyperosmolar coma. Patients should be admitted to an intensive care unit because they are critically unwell. Transfer to other institutions is not recommended until the patient has stabilised and any other causes have been ruled out
More detailsPublished - Fri, 11 Nov 2022

Created by - Rigomo Team
Alcoholic Ketoacidosis: Clinical Features, Evaluation & Treatment
Alcoholic ketoacidosis is usually seen in alcoholic patients who are forced to abruptly cease drinking alcohol after a drinking binge, but it may also be seen in first-time drinkers. Diabetes mellitus does not exist in these patients.PATHOGENESIS: The pathogenesis is uncertain. It is related to low insulin levels, reduction of available nicotinamide adenine dinucleotide, and increased ketone formation.CLINICAL FEATURES1. Patient history: The patient has recently stopped or limited alcohol consumption because of abdominal pain, nausea, and vomiting, not from a desire to stop drinking.2. Symptomsa) Diffuse abdominal pain is typically present. Pancreatitis, gastritis, and hepatitis, for example, are diseases linked to alcoholism that can induce abdominal discomfort. Other conditions unrelated to alcoholism might also produce abdominal pain (e.g., sepsis, pneumonia, pyelonephritis).b) There may be signs of alcohol withdrawal or delirium tremens.3. Physical examination findingsa) Hydration status: Dehydration occurs secondary to vomiting, diaphoresis, and decreased oral intake. The patient has tachycardia and hypotension and is critically unwell.b) Vital signs: Kussmaul respirations may be present, and the temperature may be elevated or normal.c) The range of mental states includes normal and comatose.d) Alcoholism stigmata, such as spider angiomata, may be seen.DIFFERENTIAL DIAGNOSES: An anion gap acidosis-causing condition needs to be ruled out. The most important conditions to take into account include isopropyl alcohol intoxication, hyperemesis gravidarum, hunger, cyanide poisoning, and diabetic ketoacidosis.EVALUATION1. Serum biochemical profile will establish the presence of an anion gap acidosis. A mixed disorder could also exist (e.g., metabolic ketoacidosis may occur from vomiting and respiratory alkalosis may occur from fever, sepsis, or alcohol withdrawal).2. Ketone studies: β-hydroxybutyric acid is the predominant ketone formed in alcoholic ketoacidosis. The nitroprusside test has limited use in individuals with alcoholic ketoacidosis since it only detects acetoacetate and not -hydroxybutyrate. Acetoacetate levels rise during treatment, giving the ketoacidosis a fictitious appearance of deteriorating.3. Bedside glucose determination: The level of blood sugar may be low, normal, or only slightly higher. Most individuals' blood glucose levels range from normal to elevated.THERAPY: Ketoacidosis can be reversed in 12 to 18 hours.1. Dehydration is treated with saline solutions containing glucose and thiamine. The clinical response appears to be enhanced by glucose. If inadequate oral intake is suspected, magnesium and vitamin supplements should be administered.2. Insulin: Administration of insulin is not indicated unless the patient has concomitant diabetes mellitus.3. Bicarbonate: Bicarbonate administration is under question. Most people recommend only giving bicarbonate in cases of cardiac arrest with known severe acidosis.DISPOSITION1. Admission: Patients with severe metabolic acidosis or those who are unable to tolerate oral fluids should be hospitalised. Prior to discharge, underlying or precipitating illnesses, as well as abdominal pain, must be assessed. Patients often react to therapy in 12 to 24 hours, at which point they may be released.2. Discharge: The patient might be released from the emergency room if the therapy goes well. It is crucial to closely monitor patients and refer them for alcoholism treatment.
More detailsPublished - Fri, 11 Nov 2022

Created by - Rigomo Team
Gonorrhea: Clinical Features, Evaluation & Treatment
ETIOLOGY: Gonorrhea is caused by Neisseria gonorrhoeae.Incidence: The ages of 20 and 24 have the highest frequency of the disease.CLINICAL FEATURES1. Local diseasea) Acute urethritis is the most common presentation in heterosexual men. Symptoms begin within 1 to 14 days of exposure and consist of dysuria and penile discharge. Three to ten percent of men with gonorrhea may be asymptomatic.b) Cervicitis: Primary gonorrhea in women is usually asymptomatic, and when symptoms do occur, they are usually mild and non-specific. Up to 20% of women with primary gonorrhea develop pelvic inflammatory disease, and 33% to 81% of women with the pelvic inflammatory disease have gonorrhea.c) Pharyngeal gonorrhea can be asymptomatic: The pharynx is colonized in 3% to 7% of heterosexual men, 5% to 20% of women, 10% to 25% of homosexual men, and 39% to 96% of pregnant women.d) Anorectal gonorrhea is common in both heterosexual women and homosexual men and is often asymptomatic. When symptoms occur, they are usually mild pruritus and rectal discomfort.2. Disseminated gonorrhea may complicate the disease course in 1% to 3% of patients with localized disease and is manifested most commonly as monoarticular arthritis or pustular dermatitis syndrome.DIFFERENTIAL DIAGNOSES1. Gonococcal urethritis must be differentiated from non-gonococcal urethritis caused by Chlamydia trachomatis.2. Disseminated gonorrhea: N. meningitidis infection, acute rheumatic fever, and Reiter syndrome must be ruled out. Differential diagnoses for skin lesions include syphilis, HIV infection, and condyloma acuminata.EVALUATION: Gram stain and culture of discharges are the cornerstones of diagnosis. All patients evaluated for gonorrhea should also have blood drawn for syphilis serology.THERAPY: For uncomplicated cervicitis or urethritis:1. Ceftriaxone (250 mg intramuscularly) and doxycycline (100 mg orally twice daily for 14 days, to cure possible concomitant Chlamydia infection) are the standard therapy.2. Cefixime (400 mg orally in a single dose) is no longer an accepted alternative due to resistance.3. Azithromycin, 2 g one-time dose, is an alternative for cephalosporin allergic patients.DISPOSITION1. Uncomplicated gonorrhea is managed on an outpatient basis. All sexual contacts must be identified and treated, and HIV testing should be considered by the patient with his or her primary physician at a later date.2. Patients with disseminated gonorrhea require hospitalization.
More detailsPublished - Fri, 11 Nov 2022
Created by - Rigomo Team
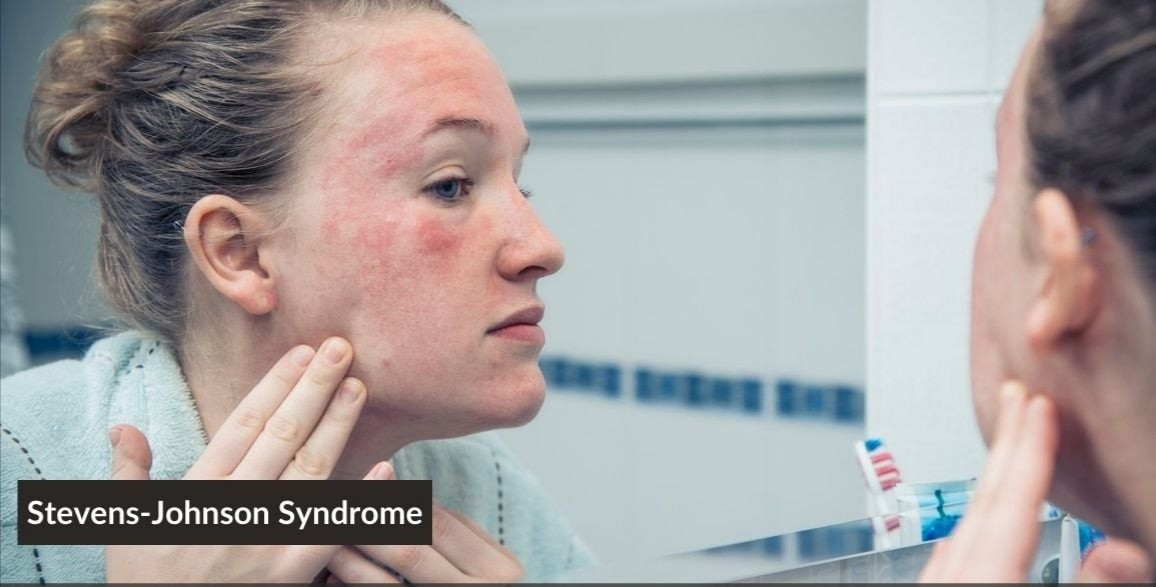
All you need to know about Stevens-Johnson Syndrome
Stevens-Johnson syndrome is a severe form of erythema multiforme, associated with a mortality rate of 10%. Complications include blindness, renal failure, meningitis, necrotizing tracheobronchitis, dehydration, secondary bacterial infection, arrhythmias, and congestive heart failure.Who is commonly affected?Children and young adults are most frequently affected by the disease. CLINICAL FEATURES1. Upper respiratory tract infection, headache, fever, hematuria, diarrhea, and arthralgias can precede the rash.2. Rash: Skin lesions are burning but not itchya) Bullae appear in 1 to 14 days on the skin and the mucous membranes of the mouth, genitalia, and anus.b) Ulcers: Corneal ulcers can lead to blindness. Ulcerative stomatitis leads to hemorrhagic crusting. Patients are unable to eat or drink and continuously drool.c) Vesicles rupture and leave denuded bases and necrotic epithelium.3. Signs of toxic epidermal necrolysis (TEN) may develop. Urinary retention can result from urethral involvement.DIFFERENTIAL DIAGNOSES include TEN and pemphigus.EVALUATION: Skin biopsy findings include necrolysis with edema and erythrocytes in the dermis.THERAPY1. Definitive treatment entails treating the cause if it can be identified (e.g., with antibiotics or termination of drug therapy). Prednisone (80 to 120 mg/day in divided doses) can be administered orally with subsequent tapering. Intravenous immunoglobulin has also been used successfully to halt the progression of TEN. It is important to note that treatment with prednisone or intravenous immunoglobulin is controversial and varies from one institution to another.2. Supportive treatmenta) Cool, wet compresses— Aluminum acetate compresses are applied to blisters.— Compresses soaked in potassium permanganate solution are applied to bullous lesions.b) Anesthetic troches, 2% viscous lidocaine, or 10% sodium bicarbonate mouthwashes can be used to soothe mouth lesions. If the patient cannot tolerate a liquid diet, he or she will require intravenous rehydration.c) Antibiotic therapy is indicated for patients with secondary bacterial infections.d) Ophthalmology consult: An ophthalmologist should be consulted.d) Urology consult: Urology should be consulted if genitourinary involvement is suspected.DISPOSITION: Patients with severe mucous membrane involvement require admission to a burn unit for reverse isolation and treatment of fluid and electrolyte imbalances.
More detailsPublished - Sat, 12 Nov 2022
Created by - Rigomo Team
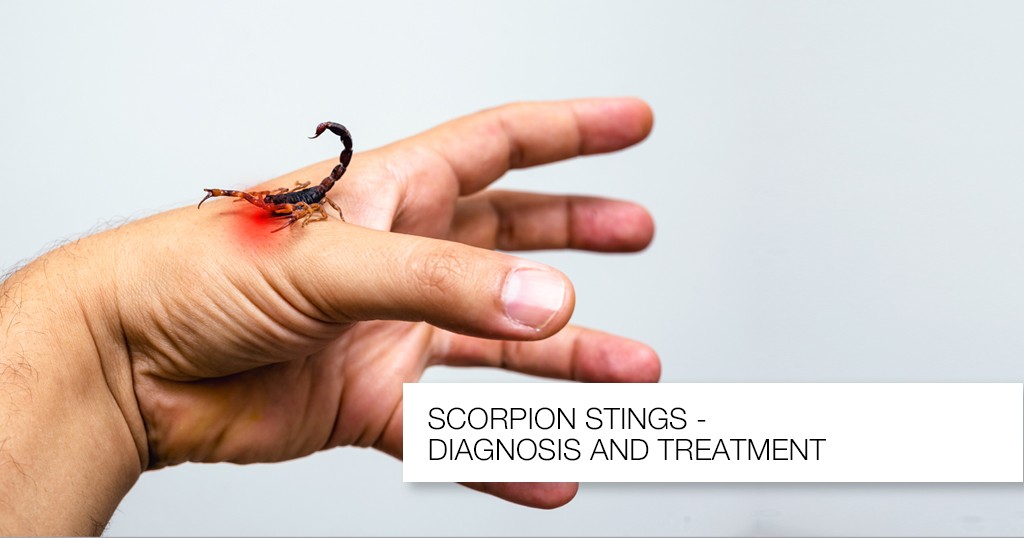
Know about Scorpion Stings
Introduction: A nocturnal arachnid that lives in the Southwest of the United States is the scorpion. It has two venom glands and a stinger in its tail. The majority of species are rather benign, and they often only create a limited reaction similar to that brought on by a bee sting. The bark scorpion (Centruroides sculpturatus) venom, on the other hand, has neurotoxic that can result in a serious reaction. This dangerous scorpion is found on trees in Arizona and New Mexico.CLINICAL FEATURES1. Local effects: The C. sculpturatus scorpion bite causes immediate, excruciating pain at the stung site, as well as swelling and ultimately, numbness. The area that was hurt is extremely sensitive, and the implicated extremity could become paralyzed.2. Systemic effects: The neurotoxin is strongly cholinergic and can cause excessive salivation, blurred vision, muscular spasms, hypertension, and respiratory difficulties.DIFFERENTIAL DIAGNOSES — Snakebite— A puncture wound or other trauma— Insect or spider bite— Drug intoxicationEVALUATION: Typically, the offending scorpion is seen or assumed by history; if safety allows the scorpion to be brought in, this is best. Due to the wide range of symptoms and quick progression, a thorough history and physical examination are necessary.THERAPY1. Pre-hospital management includes rapid transportation of the patient, application of an ice pack to the sting site, and safe transport of the scorpion for identification. When serious symptoms appear, life-saving procedures should be started.2. ED managementa) Antivenin should be administered in all cases of severe envenomation.b) Ventilatory support may be required, with intubation and oxygen for patients with severe systemic response or anaphylaxis.c) Atropine may be required to counteract the cholinergic effects; the dose is titrated to relieve the cholinergic signs.d) Benzodiazepines may be used for seizures and muscle spasms.DISPOSITION: All victims should be observed for 24 hours, especially children. Symptomatic patients should be transferred to the intensive care unit if symptoms are severe.
More detailsPublished - Sat, 12 Nov 2022

Created by - Rigomo Team
What is Pemphigus Vulgaris?
Pemphigus Vulgaris is a rare disease that affects elderly patients. The mortality rate is 10%; most deaths result from steroid complications, secondary infection, dehydration, or thromboembolism. Pemphigus Vulgaris is caused by the attachment of immunoglobulin G autoantibodies to the epidermis. It has been associated with D -penicillamine and captopril administration.CLINICAL FEATURES1. Mucosal lesions and erosions are very common. Examination of all mucosal sites is warranted.2. Non-pruritic, painful, flaccid bullae appear that rupture easily. Blisters can be extended or new bullae formed by applying firm tangential pressure on the intact epidermis.3. Weakness, weight loss, and dysphagia may be presenting complaints.DIFFERENTIAL DIAGNOSES— Erythema multiforme— Bullous impetigo— Herpes zosterEVALUATION: Biopsy of lesions shows eosinophils, intraepidermal bullae, and acantholysis. Indirect immunofluorescent staining shows immunoglobulin G antibodies. Serum titers can be followed to evaluate the effectiveness of therapy.THERAPY1. Prednisone (200 to 350 mg/day) for 5 to 10 weeks is used until the cessation of new blister formation occurs. The dosage is then reduced to 40 mg on alternative days and tapered over 1 year.2. Azathioprine (100 mg/day) is added to the regimen and the dosage is reduced over a 4- to 6-month period. Methotrexate and cyclophosphamide can be used instead of azathioprine.3. Topical analgesics (e.g., viscous lidocaine) can be used to alleviate the pain associated with oral lesions.DISPOSITION: Patients with severe cases and oral lesions may require hospital admission for intravenous hydration. Others can be treated as outpatients with close follow-up.
More detailsPublished - Tue, 15 Nov 2022
Search
Popular categories
Health and Wellness
231Skill Development
7Technology
5Community Impact
2Success story
2Strategy
1Latest blogs

DeepSchool: The Story of an Idea That Refused to Sit Still
Tue, 02 Dec 2025

Transforming Emergency Care: The Story Behind Rigomo's Revolutionary PPMMP Course
Sun, 12 May 2024

Empowering Rural Healthcare: How Pogiko's AI is Bridging the Gap in Medical Services
Thu, 25 Apr 2024
Write a public review